
Today in morning report we talked about the physical exam of a patient with psoriasis, focusing on evidence of psoriatic arthritis
Here are some tidbits that came up:
1) Psoratic Arthritis Presentation:
- 60–70% of cases, psoriasis precedes joint disease.
- 15–20% of cases, the
two manifestations appear within 1 year of each other.
- 15–20% of cases,
the arthritis precedes the onset of psoriasis
There are
five classic patterns of presentation:
- Isolated DIP arthritis
- Asymmetric oligoarthritis
- Symmetric polyarthritis (similar to RA)
- Axial disease (sacroiliitis & spondylitis)
- Arthritis mutilans
Extra-articular changes:
-
Nail changes are present in 90% of cases, there are six patterns: pitting, horizontal ridging, onycholysis, yellowish discoloration of the nail
margins, dystrophic hyperkeratosis, and combinations of these findings
- Dactylitis ("sausage digit") in >30%
- Enthesitis/tenosynovitis
- Eye: conjunctivitis or uveitis
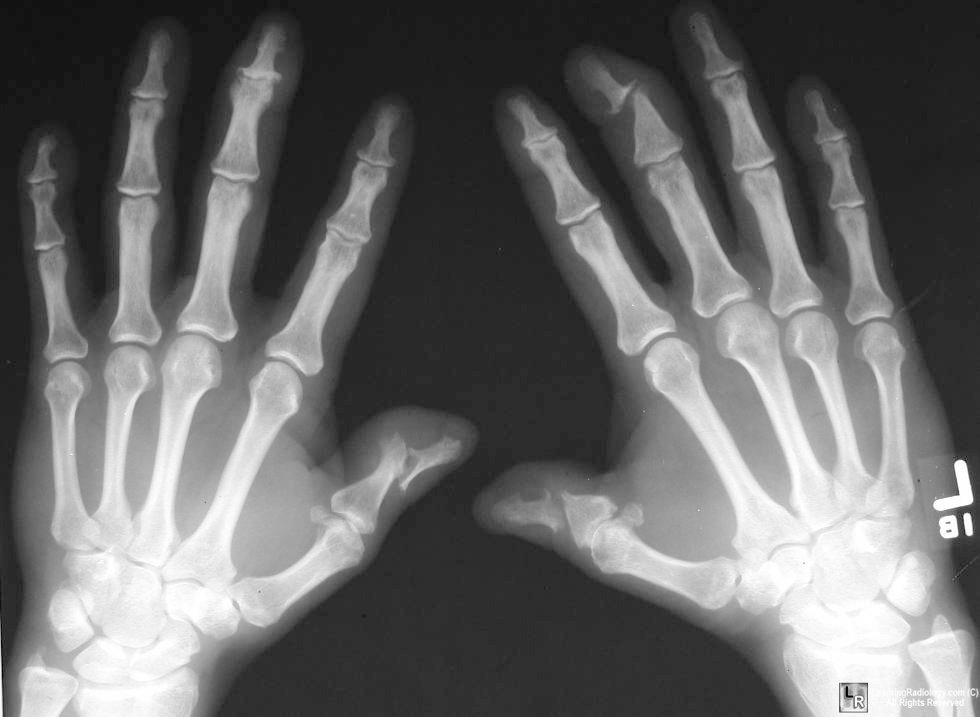
2) Findings on x-ray imaging of the hand in Psoriatic Arthritis
- DIP involvement, including the classic
"pencil-in-cup" deformity (as seen above in top image)
- marginal erosions with adjacent bony proliferation
("whiskering")
- small-joint ankylosis (loss of space)
- osteolysis of phalangeal and metacarpal
bone, with telescoping of digits (second image above)
- periostitis and proliferative new bone at
sites of enthesitis.
3) Physical Examination for Axial Involvement:
To Assess the sacroiliac joint:
- palpation along SI joint
- FABERE test: flexion, abduction, external rotation and extension of affected leg (figure 4). Test is positive if tested leg cannot be lower parallel to other leg- this will occur with hip disease, iliopsoas spasm or SI joint disease.
- lateral compression of pelvis
- Gaenslen test (below):
 To Assess mobility of lumbar spine:
To Assess mobility of lumbar spine:
- Modified Schober test: mark the point 10cm above and 5cm below the level of the dimple of Venus at the midline. Measure again with full forward flexion. This should increase to at least 20cm in flexion.
- standing back to a wall: distance from fingertip to floor on lateral flexion
4) BONUS! Diagnostic Criteria:
CASPAR criteria, a patient must have inflammatory
articular disease (joint, spine, or entheseal) with  3 points from any of the
following five categories:
3 points from any of the
following five categories:
-
Evidence of current psoriasis, a personal
history of psoriasis, or a family history of psoriasis
-
Typical psoriatic nail dystrophy observed on
current physical examination
-
A negative test result for rheumatoid factor
-
Either current dactylitisf or a history of dactylitis recorded
by a rheumatologist
-
Radiographic evidence of juxtaarticular new bone
formation in the hand or foot
That's all folks!




 3 points from any of the
following five categories:
3 points from any of the
following five categories:
